Pleural Tapping | Thoracentesis
Pleural Tapping
Thoracentesis is a procedure that is done to remove a sample of fluid from around the lung. The lung is covered with a tissue called the pleura. The inside of the chest is also lined with pleura. The space between these two areas is called the pleural space. This space normally contains just a thin layer of fluid, however, some conditions such as pneumonia, Tuberculosis, some types of cancer, or congestive heart failure, Kidney failure may cause excessive fluid to develop (pleural effusion).
To remove this fluid for evaluation (testing) or to reduce the amount of fluid, a procedure called a Thoracentesis is done.
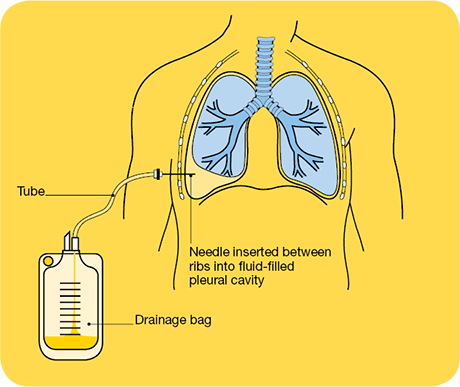
How Thoracocentesis is done?
Thoracentesis involves placing a thin needle or tube into the pleural space to remove some of the fluid. The needle or tube is inserted through the skin, between the ribs, and into the chest. This procedure may be done to remove fluid for testing or for treatment. The needle or tube is removed when the procedure is completed. If a person needs more fluid drained, sometimes the tube is left in place for a longer time.
Why Do I Need a Thoracentesis?
The most common reasons for doing a thoracentesis are:
- New pleural effusion: Thoracentesis may be done to figure out the cause of new fluid build-up in the chest.
- Infection: When an infection is suspected to be the cause of fluid build-up in the chest, thoracentesis may be done to help make a diagnosis. The fluid that is drained can be analyzed in the laboratory to identify the type of germ causing the infection and what medicines might be effective.
- Cancer: Some cancers spread to the lung or the pleura (the lining of the lung and chest wall). This can cause fluid to build up in the chest. Thoracentesis may be done to help make a diagnosis. The fluid that is drained can be examined in the laboratory to see if cancer cells are present. This type of pleural effusion is called a Malignant Pleural Effusion (MPE).
- Comfort: A large build-up of fluid can be painful and make it hard to breathe. Removing some fluid may make the person more comfortable. Eg: In the case of heart failure, kidney failure.
What are the Risks of a Thoracentesis?
Risks of having a thoracentesis are not common and are usually not serious. Some of the possible risks of thoracentesis include:
■ Pain during placement: Discomfort can result from the needle at the time it is inserted. Doctors try to lessen any pain or discomfort by giving a local numbing medicine (topical anesthetic). The discomfort is usually mild and goes away once the needle or tube is removed.
■ Bleeding: During the insertion of the needle, a blood vessel in the skin or chest wall may be accidentally nicked. Bleeding is usually minor and stops on its own. Sometimes, bleeding can cause a bruise on the chest wall. Rarely, bleeding can occur in or around the lung and may require a chest tube or surgery.
■ Collapsed lung: When the needle is being placed, it may puncture the lung. This hole may seal quickly on its own. If the hole does not seal over, air can leak out and build up around the lung. This build-up of air can cause part or all of the lung on that side to collapse (pneumothorax). If this happens, the doctor can place a chest tube between the ribs into the chest to remove the air that is leaking from the lung.
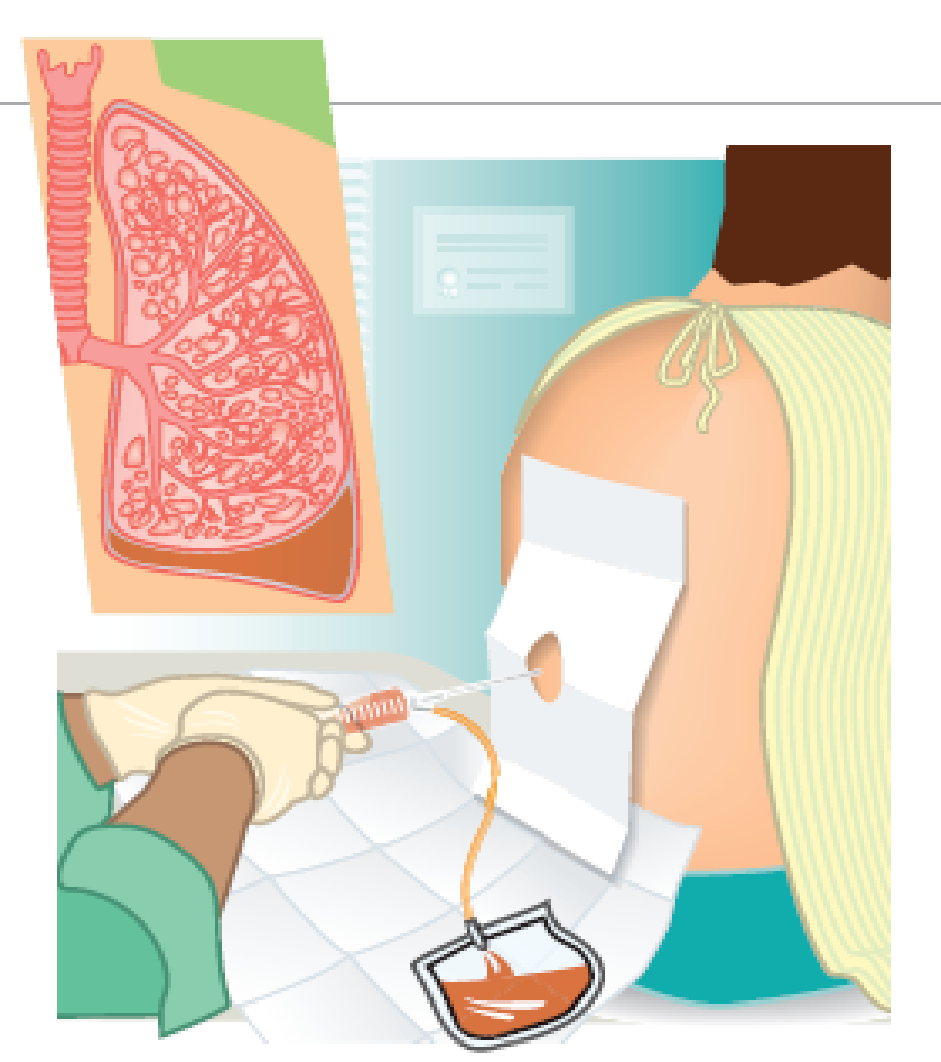
Getting ready for a Thoracentesis
Your physician will provide you with instructions about how you will need to prepare for the procedure, including taking medications prior to or the day of the procedure, following a specific diet, and so forth.
Usually, an imaging test is done to look at how much fluid is around the lungs. This may be a chest radiograph (x-ray), a chest ultrasound, and/or a chest CT (“cat-scan”) to look at where the pleural fluid is and how much is there. Sometimes the procedure is done using ultrasound guidance.
Usually, an adult or older child remains awake when a thoracentesis is done. Sometimes a person, particularly a younger child, is given medicine (a sedative) that causes sleepiness before the procedure. The skin is cleaned with a disinfectant before the needle is inserted. Sometimes a local numbing medicine (anesthetic) is injected into the skin first. The fluid may drain through the needle. When the fluid is removed, the needle is removed and a bandage is placed over the insertion site wound. The wound closes on its own without the need for stitches.
Often this procedure is done as an outpatient, though your health care provider may have you stay in the hospital for a day for observation.

Dr. Parthiv Shah
Best Pulmonologist in Mumbai
